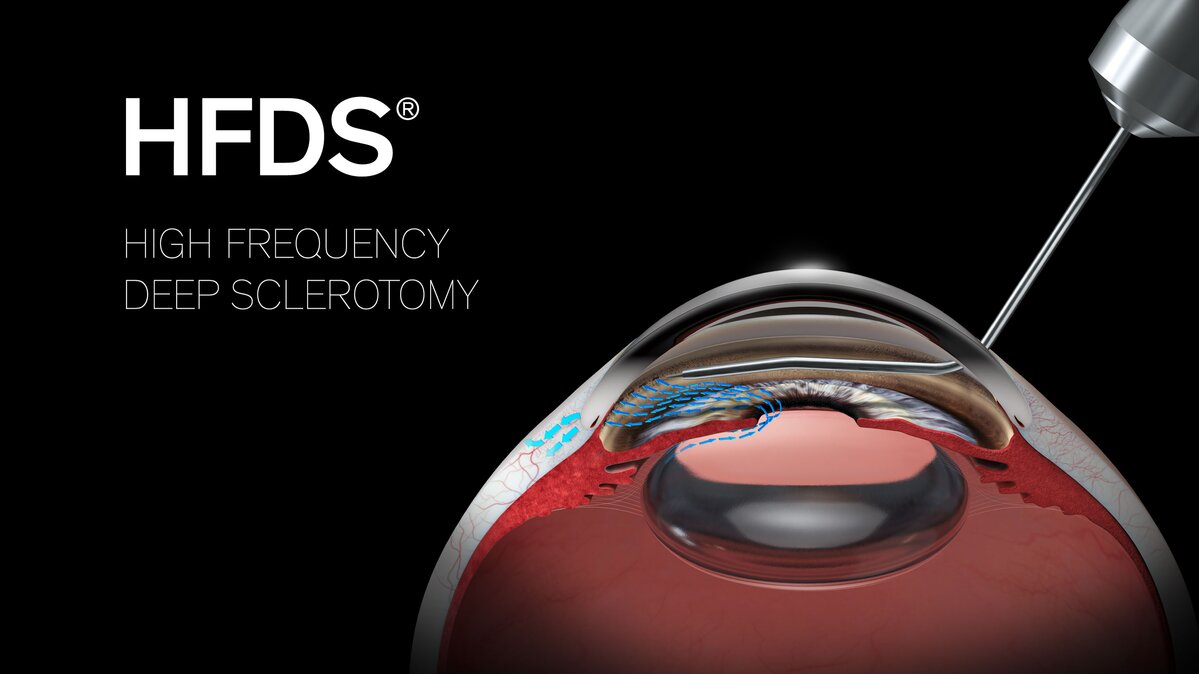
HFDS® for modern MIGS surgery
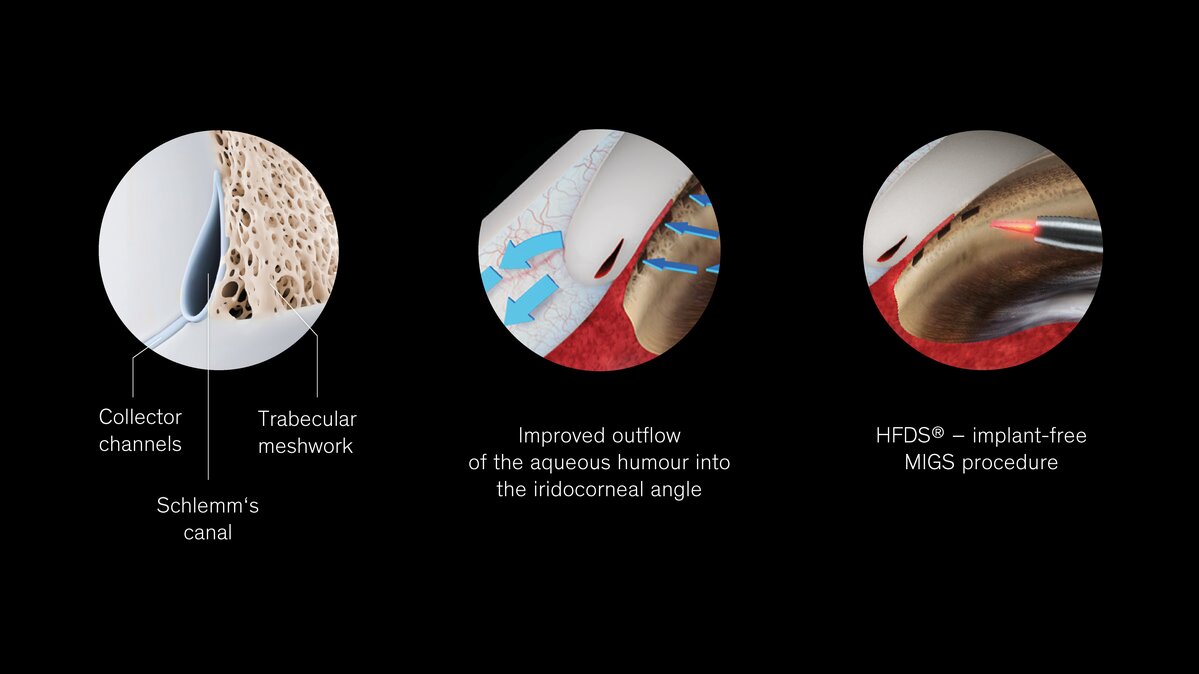
In the treatment of primary open-angle glaucoma, Oertli's HFDS ab interno MIGS technology delivers promising long-term results in the reduction of IOP 1. HFDS provides direct access from the anterior chamber to the Schlemm's canal and further into the sclera. The HFDS glaucoma tip is inserted through a 1.2 mm paracentesis and uses high-frequency diathermy to place small sclerotomy pockets in the iridocorneal angle, aiming to improve the outflow of aqueous humour. Clinical studies have confirmed a long-term and significant reduction (four years) in IOP and a reduction in anti-glaucoma medications (AGMs) 4.
How does HFDS work in glaucoma surgery?
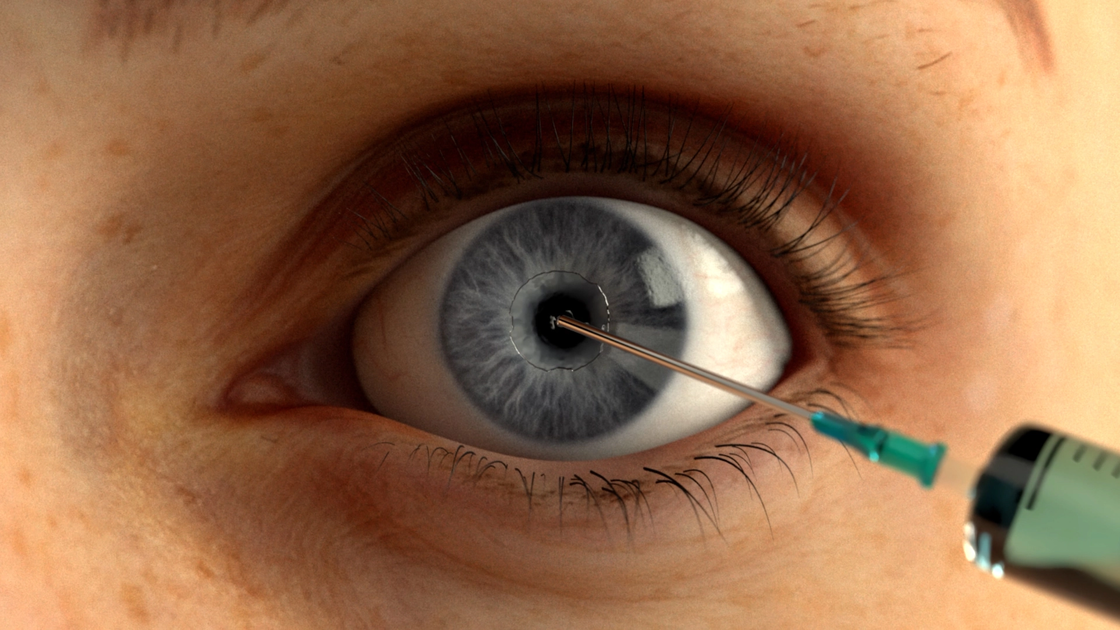
1. Anaesthesia & moistening of the cornea
The HFDS procedure can be carried out under local anaesthesia. A viscoelastic substance is applied to the cornea to ensure constant moistening.
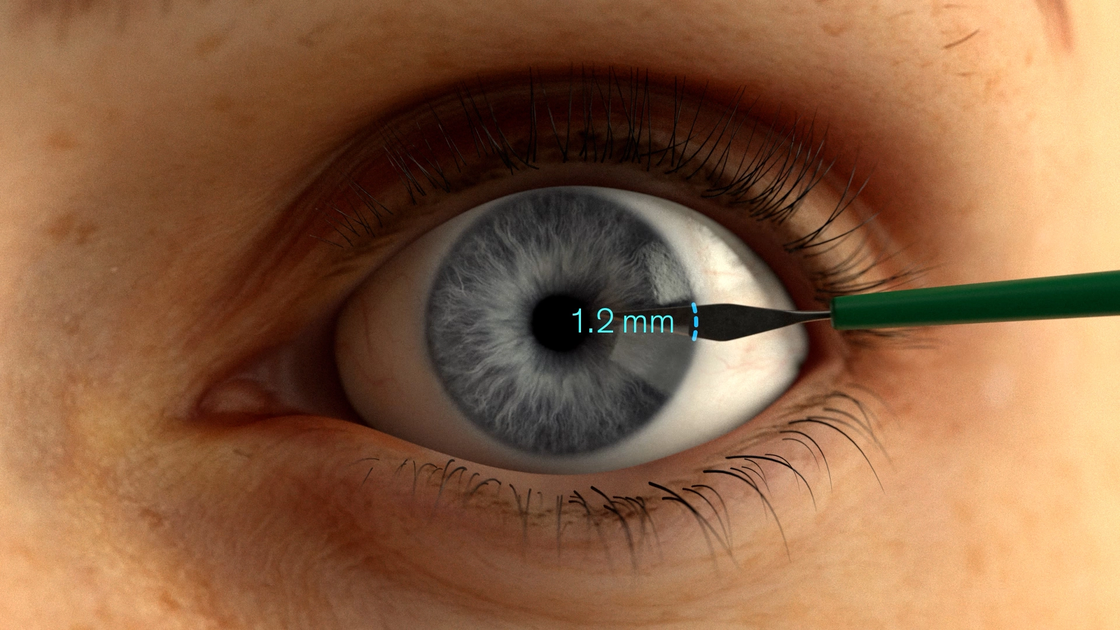
2. Incision
For nasal access, perform a 1.2 mm temporal or bitemporal incision.
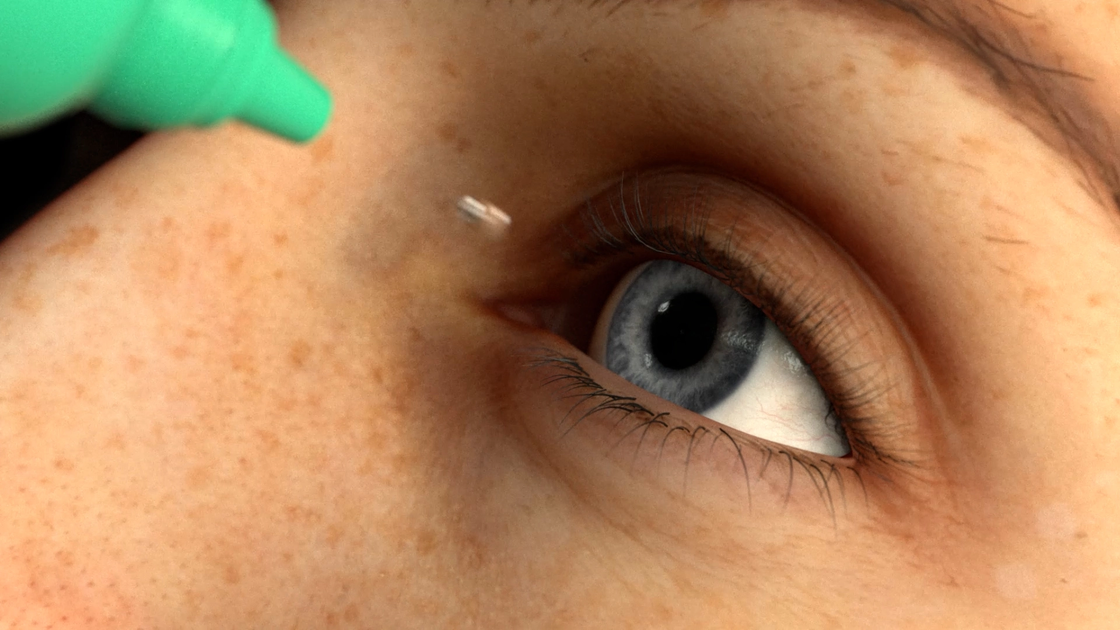
3. Induction of Miosis
Narrow the pupil using drops or an intracameral injection to protect the lens and improve visualisation of the angle.
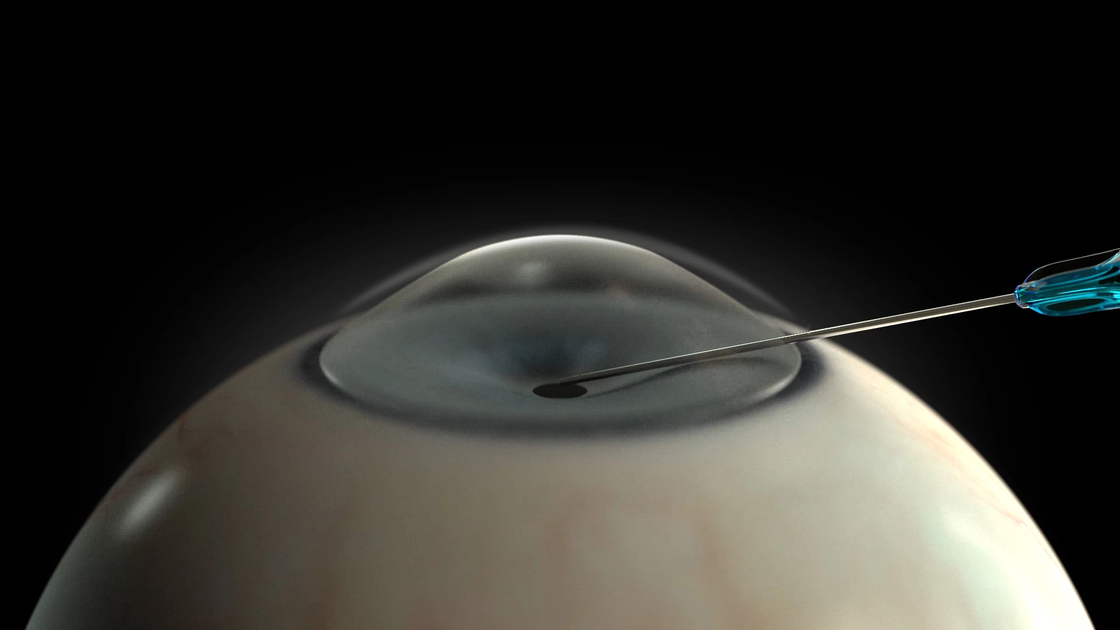
4. OVD application
Fill the anterior chamber with a high-viscosity viscoelastic substance (OVD) to maintain space and stabilise the target area.
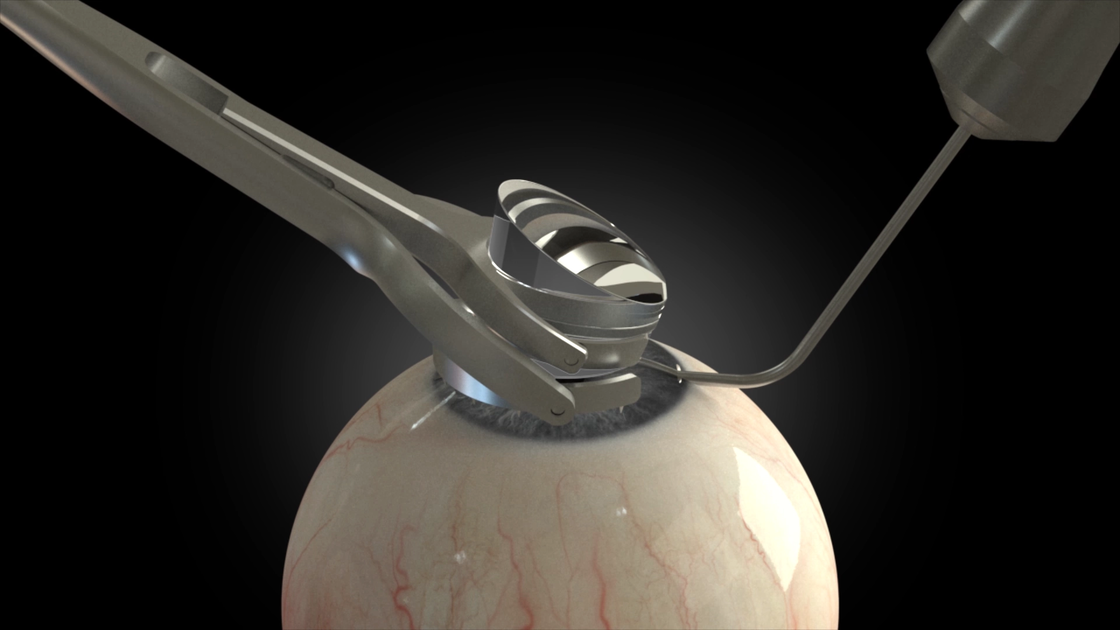
5. Visualisation of the iridocorneal angle
Apply viscoelastic substance to the cornea. Insert the tip through the incision. Place a direct or indirect goniolens. This allows for a clear view of the Schalbe's line and the pigmented trabecular meshwork.
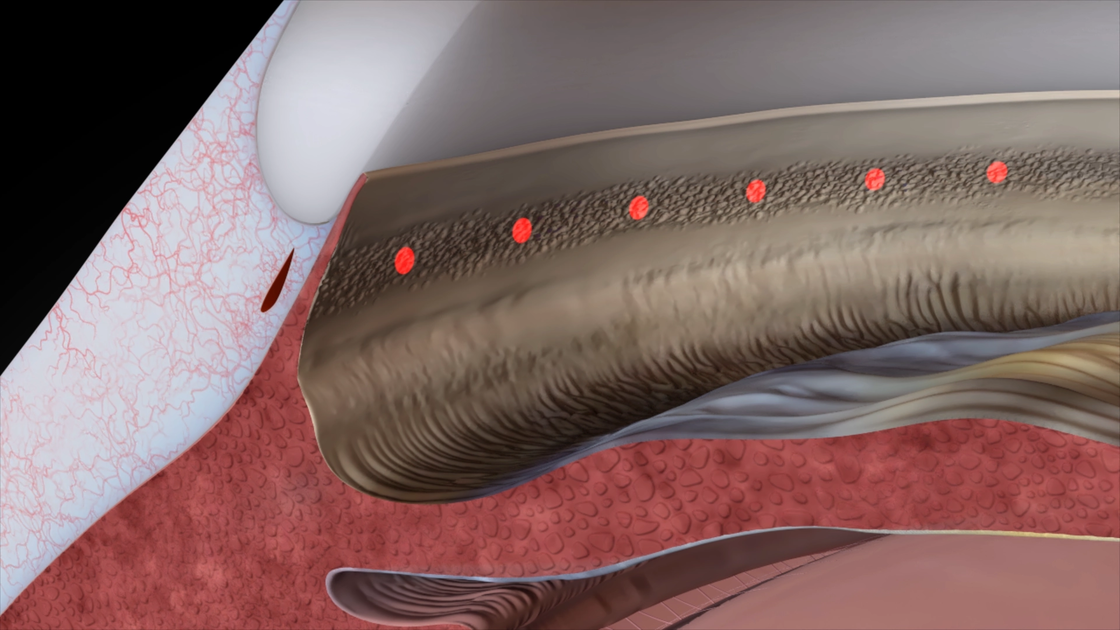
6. Positioning of the HFDS tip
Position the HFDS tip in the iridocorneal angle below Schwalbe's line and above the scleral spur at the level of the pigmented trabecular meshwork.
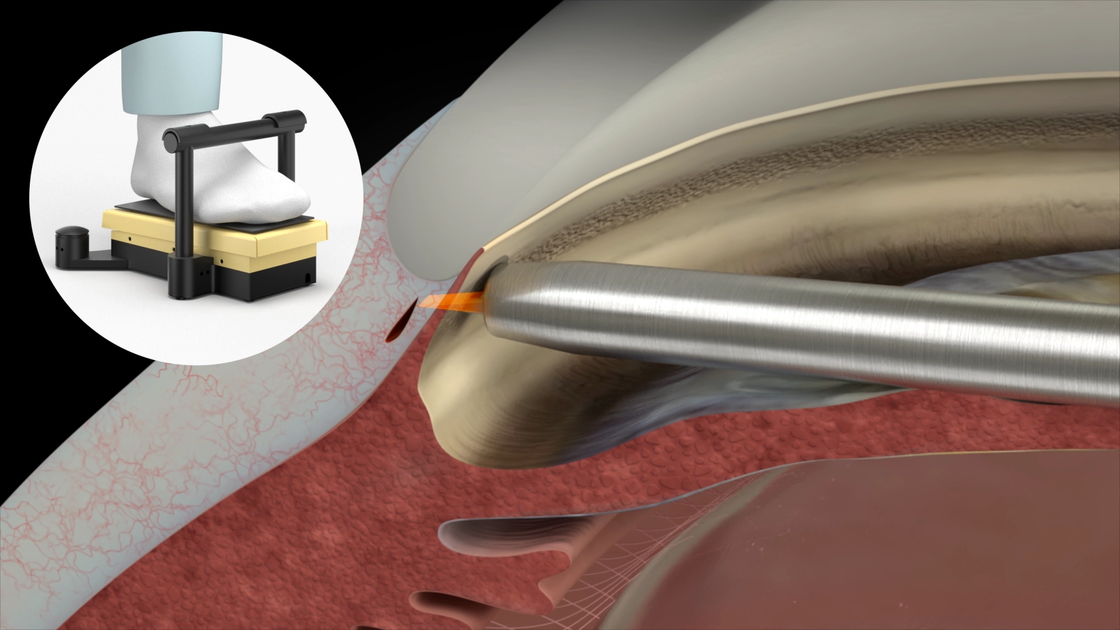
7. HFDS pockets creation
Press the pedal and simultaneously push the HFDS tip forward to create a 1 mm pocket. Using high-frequency energy, six small pockets are formed.
The HFDS procedure in detail
8. Postoperative medication
According to the recommendation of Prof. Bojan Pajic, it is advised to use Tobramycin/Dexamethasone, either as a fixed combination or separately, four times daily for four weeks, supplemented by Pilocarpine 2% eye drops for two weeks.
REDUCTION OF THE IOP
In the treatment of primary open-angle glaucoma, Oertli’s HFDS ab interno MIGS technology delivers promising long-term results in reducing IOP 1. Clinical studies have confirmed a long-term and significant reduction in IOP over a 4-year period, together with a reduction in anti-glaucoma medications (AGMs) 4.
See HFDS® in application now
What do experts say about HFDS®?
Dr Florian Sutter
Eye clinic Herisau and Appenzell, Switzerland
Length: 10 min
Dr Robert Kromer
nordBlick Eye clinic Bellevue Kiel, Germany
Length: 11 min
Do you want to know more?
-
High Frequency Deep Sclerotomy, Dr Florian Sutter, Ophthalmology Times Europe, 2022
-
Triggerfish Recording of IOP Patterns in Combined HFDS Minimally Invasive Glaucoma and Cataract Surgery, Journal of Clinical Medicine, 2021
-
Ab Interno Approach with No Implant Needed, The Ophthalmologist, 2021
-
High-Frequency Deep Sclerotomy, A Minimal Invasive Ab Interno Glaucoma Procedure Combined with Cataract Surgery: Physical Properties and Clinical Outcome, Eye Clinic Orasis, 2019
-
The Efficacy and Safety of High-Frequency Deep Sclerotomy in Treatment of Chronic Open-Angle Glaucoma Patients, Research Institute of Ophthalmology Cairo, Cairo University Faculty of Medicine, 2019
-
Ab-Interno Deep Sclerotomy in Eight Simple Steps, Cataract & Refractive Surgery Today Europe, 2017
-
The Future Way of Phaco & MIGS Surgeries - Highlights from ESCRS Satellite Symposium, The Ophthalmologist, 2015
-
HFDS Glaucoma Procedure, Dr. Bojan Pajic, European Opthalmic Review, 2012
-
New Minimally Invasive, Deep Sclerotomy ab interno Surgical Procedure for Glaucoma, Six Years of Follow-up, Dr. Bojan Pajic, Journal of Glaucoma, 2011
HFDS in glaucoma surgery
Learn more about about the instruments for glaucoma surgery.
The HFDS DryLab KIT
With the compact, mobile and flexible training tool, we provide a more impactful introduction into HFDS than ever before.
Cataract surgery
Innovations such as HF capsulotomy and easyPhaco are developments that aim to make cataract surgery faster and more efficient.
More about cataract